Many people find that using self help techniques such as changing positions, relaxation, showering and massage are all they need to cope with labour pain. Some people find that they need or want more help to cope with labour.
Other pain relief options including medication are available. It is important to know how they can help you as well as possible side effects for you, your baby and your recovery. Your healthcare provider can help you with decisions about pain relief options in labour. We encourage you to find out more about these options before your labour starts.
Medical options
TENS (external)
- Stands for Transcutaneous Electrical Nerve Stimulation
- Four electrode pads attach to the lower back and give a rhythmic, tingling, pulsing sensation
- The electrodes are attached by wires to a hand held unit, which the labouring person uses to change the strength and frequency of the sensations as needed
- TENS uses the principles of the ‘gate theory of pain relief’ – sensory signals reach the brain faster than pain signals and the brain perceive pain signals as weaker than they really are because they are “masked” by the sensory signals
Benefits
- Can provide good pain relief in early labour
- Can be used at home
- The labouring person is in control of the strength of the sensation
- It is a distraction from the pain from the contractions
- The labouring person is able to move around freely
- No negative risks or side effects on labour or on baby
Disadvantages/Risks
- The batteries will need to be changed every 4-6 hours during labour to maintain effectiveness
- Not as effective in active labour as early labour for some people
- Can’t be used in the bath or shower
- The TENS machine needs to be rented or purchased before labour starts, as it is not usually available in hospitals and birth centres
Other Information and Support Tips
- TENS works best if it is applied in early labour so you would need to have the unit before you go into labour
- There are specific labour TENS machines that can be rented or purchased online. Some medical supply stores may also have them
- The TENS machine will come with instructions giving details on how to use the machine and how to apply the electrodes to your back
- A support person can apply the TENS machine to your back in early labour. Remember to change the batteries throughout labour and continue to offer other comfort and support methods.
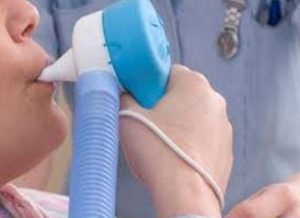
Entonox (inhaled)
- “Laughing Gas” (a mixture of 50% nitrous oxide and 50% oxygen)
- Self administered during a contraction, through a mask or mouthpiece
- Can be used in any stage of labour
- Lasts the length of the contraction
Benefits
- Can provide good pain relief at any stage in labour
- No impact on recovery or breastfeeding
- You control the amount you receive
- Can be used with other methods of pain control
- Helps you focus on breathing
- Little effect on baby
- Doesn’t increase the likelihood of other medical interventions
Disadvantages/Risks
- May cause dizziness, numbness or tingling, or nausea
- Doesn’t completely eliminate pain
Other Information and Support Tips
- Breathing Entonox will make the labouring person’s mouth dry so be sure to offer ice chips, sips of water, and lip balm between contractions
- Remind the labour person to take slow deep breaths into the mask from the start of contractions to ensure they get enough medication, then to breath room air after the peak and between contractions to exhale the gas from their lungs
- Continue to use comfort techniques such as massage and touch
Narcotics (intravenous or intramuscular)
- Pain medication such as Morphine ®, Fentanyl ®
- Usually given by injection or intravenous (IV/drip)
Benefits
- Can be used throughout labour
- IV (injected into a vein) works in 2 to 3 minutes; lasts 1 to 2 hours
- IM (injected into muscle) works in 20 to 30 minutes; lasts 2 to 3 hours
- Decreases the perception of pain felt in labour
- May help you to relax and let you get some rest in between contractions
- Doesn’t interfere with the urge to push or increase the need for further medical interventions
- Short acting
Disadvantages/Risks
- May cause dizziness, nausea, drowsiness
- May make your baby drowsy and may affect their breathing and breastfeeding initiation
- Does not eliminate all the pain
- May slow labour if given before active labour is well established
- Short acting
Other Information and Support Tips
- The medication may make the labouring person dizzy and feel uncoordinated so you may need to help them change positions in bed
- Continue to use comfort measures such as massage and touch. Wipe their face and offer sips of water between contractions
- A person using narcotics in labour may be very sleepy and thus unaware that a contraction has started until it is at its peak. This makes it difficult to use coping and comfort techniques effectively. You can let them know a contraction is starting if you keep one hand on their abdomen to feel for the uterus beginning to tighten. The nurse can help to show you how to do this
- After the birth, keep baby skin to skin, with either parent, as much as possible to help with breastfeeding
- When the medication wears off the labouring person can choose to either have additional doses or allow it to wear off to move around freely again and make use of other comfort strategies, e.g. the shower
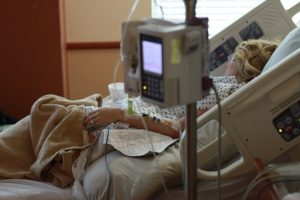
Epidural
- Uses an anesthetic, which numbs nerves, or a combination of anesthetic and narcotic
- A needle is inserted into the space surrounding the spine, a tube is then inserted through the needle, the needle is removed and medication is given through the tube. The tube stays in place until after the baby is born
- The tube may be hooked to a pump which regulates the amount of medication
- You may have a patient control button to allow you to give yourself more medication when you need it
Benefits
- Can be used throughout labour
- Can provide the most effective pain relief
- A low-dose block can sometimes give effective pain relief and still let you move around with help (this is not always possible and you may have to stay in bed)
- A full block completely blocks feeling from waist to knees
- Top-ups (more medication) are easily given, and often this can be controlled by the labouring person
- Pain relief can be achieved in 2 to 3 contractions
- You can be awake if a cesarean birth is needed
Disadvantages/Risks
- You may develop a fever in labour and the need for more bloodwork and monitoring for you and your baby
- May slow or stop labour, especially if given before active labour is established. If contractions slow down, oxytocin may be needed to stimulate labour, this may in turn lead to other medical interventions
- An epidural may lower your blood pressure. An IV will be started before the epidural is given
- A decrease in your blood pressure could slow the baby’s heart rate, which make increase the risk of needing other interventions
- Sometimes the dose needed to give pain relief causes weakness of the legs and you may have to stay in bed
- Pain relief may be “patchy” (which means you may still feel pain in some areas). This can usually be fixed
- You may lose bladder tone temporarily and you may need to have a catheter (a tube in your bladder) during labour to drain the urine
- You may lose the urge to push with contractions. Your nurse can direct you to push with contractions. Forceps or vacuum extraction is more likely to be needed for the birth of your baby, which can lead to a longer recovery time
- You may experience shivering and/or itchiness
- You may have a severe headache after delivery that can last up to a week
- Minor back pain (bruised feeling) at the site of the epidural is common and usually goes away within a week
- The medication may impact the baby’s initial attempts at breastfeeding
- Very rarely, breathing problems, infection, nerve damage or paralysis may occur
Other Information and Support Tips
When epidural medications are given, you will be attached to an electronic fetal heart rate monitor. The monitor will be placed around your abdomen again for routine monitoring or if there is a concern about your baby, if you receive oxytocin to stimulate your labour or if you receive extra doses of epidural medication. Most women who want an epidural can have one. There are some medical conditions that prevent a woman from having an epidural. These conditions can be discussed with your healthcare provider ahead of time.
Supporting Someone who has Epidural Anesthesia
- Help them to spend about 20 – 30 minutes in each of these positions to help the baby move through the pelvis: Side-lying (left), semi-prone (left), hands and knees or kneel over a birth ball, semi-prone (right), side-lying (right), semi-sitting
- Encourage them to change position every 20 -30 minutes, as much as they are able. This will decrease the chances that the baby will remain in an unfavorable position. Depending on the type and level of anesthesia, a labouring person may be able to stand and walk to the bathroom with support or may only be able to turn over in bed with a lot of assistance
- Be aware of their position in bed. Do they look like they would be comfortable staying in that position for an hour? A person with epidural anesthesia may not be aware of their body and may remain in a position that they would normally change because they are uncomfortable. If they remain in a poor position for a long period it could cause back, shoulder or hip pain in the postpartum period
- Continue with comfort measures such as offering sips of fluid, wiping the neck and face with a cool cloth, or massaging their hands, shoulders, scalp or face
- Ask to delay pushing until the baby has progressed down in the pelvis and the labouring person feels an urge to push.
- In the postpartum period, keep baby skin to skin as much as possible to help baby with breast/chestfeeding